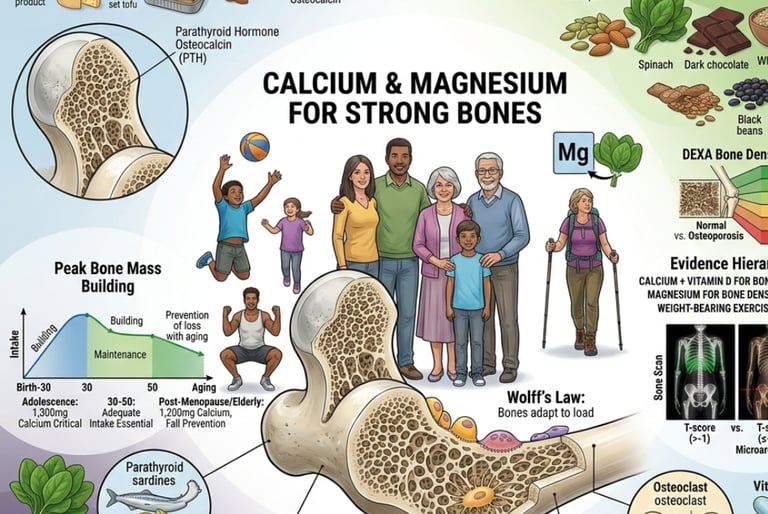
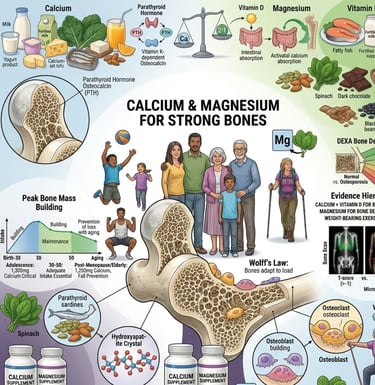
The Benefits of Calcium and Magnesium for Bone Health: Evidence-Based Guide
54 million Americans have osteoporosis/low bone density. Calcium+vitamin D: VERY STRONG evidence. Magnesium critical. Balance matters. Exercise essential.(The Benefits of Calcium and Magnesium for Bone Health)
by WellnessWithForever
3/5/202622 min read
The Benefits of Calcium and Magnesium for Bone Health: Evidence-Based Guide
By WellnessWithForever 5 March 2026: This post might contain affiliate links.
Osteoporosis affects over 10 million Americans, with another 44 million having low bone density (osteopenia), placing them at increased fracture risk. Hip fractures alone result in 300,000 hospitalizations annually, with significant mortality and loss of independence. Yet bone health is largely preventable through nutrition, exercise, and lifestyle—with calcium and magnesium playing critical but often misunderstood roles. This guide examines the evidence for how these minerals support bone health, optimal intake, the importance of balance, and comprehensive strategies for building and maintaining strong bones throughout life.
Important Medical Disclaimer: Osteoporosis and bone health disorders require professional medical diagnosis and treatment. Very high calcium supplementation may increase cardiovascular risk in some individuals. Magnesium supplements interact with certain medications (antibiotics, bisphosphonates, diuretics). Some people should not take calcium supplements without medical supervision (history of kidney stones, hypercalcemia, certain heart conditions). Bone health requires comprehensive assessment including bone density testing, fracture risk evaluation, and screening for underlying conditions (vitamin D deficiency, hyperparathyroidism, celiac disease, hyperthyroidism). This information is educational and does not replace professional medical care. Always consult healthcare providers before starting supplements, especially if you have medical conditions or take medications.
Key Takeaways
99% of body's calcium stored in bones and teeth (structural foundation)
60% of bone mineral content is calcium; magnesium also critical for bone matrix
Calcium has VERY STRONG evidence for bone health when combined with vitamin D
Magnesium has MODERATE to STRONG evidence for bone density and fracture risk
Calcium-magnesium BALANCE matters (optimal ratio approximately 2:1)
Dietary calcium superior to supplements (better absorption, no cardiovascular concerns)
Vitamin D essential for calcium absorption (calcium supplementation without adequate vitamin D ineffective)
Weight-bearing exercise critical (builds bone density that nutrition alone cannot)
Peak bone mass achieved by age 30 (prevention starts early!)
Bone remodeling continues throughout life (never too late to improve bone health)
Understanding Bone Health and Osteoporosis
Evidence quality: VERY STRONG for all bone biology and osteoporosis mechanisms
Bone Structure and Function
What bones are:
Living tissue constantly being remodeled
Provide structural support, protect organs, enable movement
Store minerals (99% body calcium, 85% phosphorus, 50-60% magnesium)
Produce blood cells (bone marrow)
Regulate mineral homeostasis (release calcium into blood when needed)
Bone composition:
Mineral component (~65% of bone weight): Calcium hydroxyapatite crystals providing hardness and strength
Organic matrix (~35%): Collagen (primarily type I) providing flexibility and framework, non-collagen proteins (osteocalcin, osteopontin, others)
Cells: Osteoblasts (bone-building cells), osteoclasts (bone-resorbing cells), osteocytes (mature bone cells regulating remodeling)
Bone Remodeling Process
Evidence quality: VERY STRONG
Continuous lifelong process:
Old bone constantly being broken down (resorption) and new bone formed (formation)
Approximately 10% of skeleton remodeled annually in adults
Balanced in healthy young adults (formation = resorption)
Imbalanced with aging (resorption > formation → net bone loss)
The remodeling cycle:
Step 1: Activation
Signals trigger remodeling (mechanical stress, hormones, damage, mineral needs)
Osteoclast precursors recruited to bone surface
Step 2: Resorption
Osteoclasts dissolve mineral and digest organic matrix
Creates resorption cavity
Lasts 2-4 weeks
Step 3: Reversal
Osteoclasts undergo apoptosis (programmed cell death)
Transition to formation phase
Step 4: Formation
Osteoblasts fill cavity with new bone matrix (osteoid)
Matrix mineralizes over 3-4 months
Osteoblasts become embedded as osteocytes or return to bone surface
Factors affecting balance:
Promote formation: Weight-bearing exercise, adequate calcium/vitamin D/protein, estrogen, growth hormone, IGF-1
Increase resorption: Physical inactivity, calcium/vitamin D deficiency, menopause (estrogen loss), aging, glucocorticoids, smoking, excessive alcohol
Peak Bone Mass and Age-Related Changes
Peak bone mass:
Maximum bone density achieved typically by age 25-30
90% accumulated by age 18 in girls, age 20 in boys
Determined by genetics (60-80%), nutrition, exercise, hormones
Higher peak bone mass = lower osteoporosis risk later
Age-related bone loss:
Begins around age 30-35 (slow gradual loss)
Accelerates dramatically in women at menopause (estrogen loss increases osteoclast activity)
Women can lose 20% of bone density in 5-7 years post-menopause
Men experience slower gradual loss (no sudden hormonal drop)
By age 70-80, significant bone loss has occurred in most people
Osteoporosis and Fracture Risk
Osteoporosis definition:
Bone density more than 2.5 standard deviations below young adult mean (T-score ≤ -2.5)
Characterized by low bone mass and deteriorated bone microarchitecture
Dramatically increased fracture risk
Osteopenia:
Bone density 1-2.5 standard deviations below young adult mean (T-score -1 to -2.5)
Intermediate risk (higher than normal, lower than osteoporosis)
Often precursor to osteoporosis without intervention
Fracture consequences:
Hip fractures: 20-30% mortality within 1 year, 50% never regain independence
Vertebral fractures: Chronic pain, height loss, kyphosis (hunched posture), reduced lung function
Wrist fractures: Functional impairment, reduced quality of life
Economic burden: $19 billion annually in US
Risk factors:
Non-modifiable: Age, female gender, family history, small frame, ethnicity (Caucasian, Asian higher risk)
Modifiable: Calcium/vitamin D deficiency, physical inactivity, smoking, excessive alcohol, low body weight, medications (glucocorticoids, some antiseizure drugs, PPIs long-term)
Calcium for Bone Health
Evidence quality: VERY STRONG when combined with vitamin D
Calcium's Role in Bones
Structural component:
99% of body calcium stored in bones and teeth
Calcium phosphate crystals (hydroxyapatite) provide bone hardness and strength
Approximately 60% of bone mineral content is calcium
Continuous exchange between bone calcium and blood calcium
Functions beyond structure:
Blood calcium regulation (bones release calcium when blood levels drop)
Muscle contraction, nerve transmission, blood clotting, hormone secretion
Maintaining blood calcium is PRIORITY (body will sacrifice bone calcium to maintain blood levels)
Evidence for Calcium and Bone Health
Bone density:
STRONG to VERY STRONG evidence calcium intake associated with higher bone mineral density
Effects most pronounced when combined with adequate vitamin D
Greatest benefits during bone-building years (childhood, adolescence, young adulthood)
Continues to benefit bone density in older adults when adequate vitamin D present
Fracture risk:
MODERATE to STRONG evidence calcium plus vitamin D reduces fracture risk
Meta-analyses show 15-30% reduction in total fractures, 20-30% reduction in hip fractures
Evidence strongest for elderly populations
Calcium ALONE (without vitamin D) shows minimal fracture reduction
Vitamin D status critical for calcium to be effective
Important nuance:
Dietary calcium appears superior to supplemental calcium
High-dose calcium supplements (>1,000mg daily) may increase cardiovascular risk in some people (evidence mixed but concerning)
Food sources provide calcium plus other bone-supporting nutrients (protein, vitamin K, magnesium, etc.)
Calcium Requirements
Evidence quality: STRONG for established recommendations
Recommended Dietary Allowances (RDAs):
Children and adolescents:
1-3 years: 700mg daily
4-8 years: 1,000mg daily
9-18 years: 1,300mg daily (critical bone-building period!)
Adults:
19-50 years: 1,000mg daily (men and women)
51-70 years: 1,000mg daily (men), 1,200mg daily (women post-menopause)
71+ years: 1,200mg daily (both genders)
Pregnancy and lactation:
14-18 years: 1,300mg daily
19-50 years: 1,000mg daily
Upper limits (safety):
Adults: 2,500mg daily (ages 19-50), 2,000mg daily (51+)
Exceeding may increase kidney stone risk, cardiovascular concerns
Dietary Calcium Sources
Evidence quality: STRONG for calcium content and bioavailability
Dairy products (best absorbed):
Milk (1 cup): 300mg
Yogurt (1 cup): 300-450mg
Cheese, hard (1 oz): 200-300mg
Cottage cheese (1 cup): 125-150mg
Fortified foods:
Fortified plant milk (almond, soy, oat—1 cup): 300-450mg (check labels!)
Fortified orange juice (1 cup): 300mg
Fortified cereals: varies 100-1,000mg per serving
Vegetables (moderate absorption due to oxalates in some):
Collard greens, cooked (1 cup): 268mg
Turnip greens, cooked (1 cup): 197mg
Kale, cooked (1 cup): 94mg
Bok choy, cooked (1 cup): 158mg
Broccoli, cooked (1 cup): 62mg
Other sources:
Canned sardines with bones (3 oz): 325mg
Canned salmon with bones (3 oz): 180mg
Tofu, calcium-set (1/2 cup): 250-750mg (varies by brand)
Almonds (1 oz): 75mg
White beans (1 cup): 161mg
Bioavailability considerations:
Dairy: ~30% absorbed (best)
Low-oxalate vegetables (kale, bok choy, broccoli): ~50% absorbed
High-oxalate vegetables (spinach, beet greens, Swiss chard): <5% absorbed (oxalates bind calcium)
Fortified foods: varies 25-35%
Calcium Supplementation
When supplements may be appropriate:
Dietary intake consistently inadequate despite efforts
Lactose intolerance, dairy allergy
Vegan diet without adequate fortified foods
Medical conditions affecting absorption (celiac, IBD, gastric bypass)
Certain medications reducing absorption (PPIs long-term)
Types of calcium supplements:
Calcium carbonate:
40% elemental calcium (highest)
Requires stomach acid for absorption (take WITH meals)
May cause gas, constipation in some
Least expensive
Examples: TUMS, Caltrate
Calcium citrate:
21% elemental calcium
Absorbed without stomach acid (can take without food)
Better for older adults, people on PPIs, post-gastric bypass
Less likely to cause constipation
More expensive
Examples: Citracal
Dosing guidelines:
Take no more than 500-600mg elemental calcium per dose (absorption decreases with larger doses)
Divide doses throughout day if taking >600mg total
Take separately from iron supplements, thyroid medication, some antibiotics (can interfere with absorption)
Provides balanced calcium support with complementary nutrients
Includes vitamin D for calcium absorption (addressing the essential partnership)
Contains magnesium supporting proper calcium-magnesium balance
Di-calcium phosphate and calcium carbonate sources
Take with meals for optimal absorption
Combines with Forever Daily for comprehensive mineral support
IMPORTANT cardiovascular concerns:
Some studies suggest calcium supplements (>1,000mg daily, particularly without vitamin D) may increase cardiovascular events (heart attack, stroke) in some populations
Evidence MIXED but concerning enough that many experts now recommend prioritizing DIETARY calcium over high-dose supplements
If supplements needed, take lowest effective dose, always with vitamin D, preferably spread throughout day with meals
Forever Calcium includes vitamin D and magnesium addressing these concerns through balanced formulation
Magnesium for Bone Health
Evidence quality: MODERATE to STRONG
Magnesium's Role in Bones
Structural component:
50-60% of body magnesium stored in bone
Integral part of bone mineral matrix
Influences hydroxyapatite crystal size and quality
Functional roles in bone metabolism:
Required for vitamin D metabolism (conversion to active form)
Required for parathyroid hormone (PTH) function (regulates calcium homeostasis)
Stimulates osteoblast activity (bone formation)
Regulates osteoclast activity (bone resorption)
Affects bone mineralization quality
Critical insight: Magnesium deficiency impairs calcium metabolism even with adequate calcium intake!
Evidence for Magnesium and Bone Health
Bone density:
MODERATE to STRONG evidence higher magnesium intake associated with higher bone mineral density
Particularly important for postmenopausal women
Some studies show magnesium supplementation increases bone density in osteopenic/osteoporotic women
Fracture risk:
MODERATE evidence higher magnesium intake associated with lower fracture risk
Effects may be particularly pronounced in magnesium-deficient individuals
Works synergistically with calcium and vitamin D
Observational studies:
Framingham Heart Study: Higher magnesium intake associated with higher bone density in men and women
Women's Health Initiative: Higher dietary magnesium associated with higher bone density
Multiple studies show inverse relationship between magnesium intake and fracture risk
Intervention studies:
Some trials show magnesium supplementation (250-750mg daily) increases bone density
Effects most pronounced in deficient individuals
Often combined with calcium and vitamin D in studies (synergistic effects)
Magnesium Requirements
Recommended Dietary Allowances (RDAs):
Children:
1-3 years: 80mg daily
4-8 years: 130mg daily
9-13 years: 240mg daily
14-18 years: 410mg (boys), 360mg (girls)
Adults:
19-30 years: 400mg (men), 310mg (women)
31+ years: 420mg (men), 320mg (women)
Pregnancy:
14-18 years: 400mg daily
19-30 years: 350mg daily
31-50 years: 360mg daily
Upper limit from supplements: 350mg daily (additional to dietary magnesium)
Dietary Magnesium Sources
Evidence quality: STRONG for magnesium content
Nuts and seeds (richest sources):
Pumpkin seeds (1 oz): 150mg
Almonds (1 oz): 80mg
Cashews (1 oz): 75mg
Brazil nuts (1 oz): 107mg
Legumes:
Black beans (1 cup cooked): 120mg
Edamame (1 cup): 100mg
Lima beans (1 cup): 80mg
Whole grains:
Brown rice (1 cup cooked): 85mg
Quinoa (1 cup cooked): 118mg
Oatmeal (1 cup cooked): 60mg
Whole wheat bread (2 slices): 45mg
Dark leafy greens:
Spinach, cooked (1 cup): 157mg
Swiss chard, cooked (1 cup): 150mg
Other sources:
Dark chocolate (1 oz, 70-85% cacao): 65mg
Avocado (1 medium): 58mg
Banana (1 medium): 32mg
Salmon (3 oz): 26mg
Note: Most Americans do NOT consume adequate magnesium (dietary surveys show average intake below RDA)
Magnesium Supplementation
Forms of magnesium:
Magnesium citrate:
Well absorbed
Mild laxative effect (can help constipation or cause diarrhea depending on dose)
Good for general supplementation
Magnesium glycinate:
Very well absorbed
Least likely to cause diarrhea
Calming effects (glycine is inhibitory amino acid)
Best for people sensitive to GI effects
Magnesium oxide:
Poorly absorbed (~4%)
Strong laxative effect
Often used for constipation, NOT ideal for bone health supplementation
Magnesium malate:
Well absorbed
May support energy production
Dosing for bone health:
200-400mg daily (elemental magnesium)
Take with meals to improve absorption and reduce GI effects
Start low and increase gradually if needed
Divide doses if taking >200mg
Comprehensive multivitamin providing balanced mineral support
Includes magnesium along with calcium, vitamin D, and other bone-supporting nutrients
Vitamin K, boron, and trace minerals supporting bone metabolism
Convenient single daily supplement for foundational nutrition
Combines with Forever Calcium for comprehensive bone health approach
Provides baseline nutrient support even on days when dietary intake suboptimal
Cautions:
Can cause diarrhea at high doses (reduce dose if occurs)
Interacts with certain antibiotics (tetracyclines, quinolones), bisphosphonates (take 2+ hours apart)
Caution with kidney disease (impaired excretion)
The Calcium-Magnesium Balance
Evidence quality: MODERATE to STRONG for importance of ratio
Why Balance Matters
Physiological relationship:
Calcium and magnesium have antagonistic and complementary roles
Both required for bone health, muscle function, nerve transmission
Imbalance can impair function of both
In bones:
Both incorporated into bone mineral matrix
Magnesium required for calcium utilization
Excess calcium without adequate magnesium may impair bone quality
In soft tissues:
Calcium promotes muscle contraction, magnesium promotes relaxation
Calcium can displace magnesium when ratio severely imbalanced
May contribute to muscle cramps, tension, cardiovascular issues
Optimal Calcium-Magnesium Ratio
Traditional recommendation: Approximately 2:1 calcium to magnesium
Reasoning:
Based on bone mineral composition
Typical intake from whole foods diet
Supports both minerals' functions
Modern considerations:
Many Americans consume HIGH calcium (especially with supplements/fortified foods) but LOW magnesium
May result in ratios of 4:1, 5:1, or even higher
Some experts now recommend closer to 2:1 or even 1:1 for people with very high calcium intake
Practical application:
If consuming 1,000mg calcium daily → aim for 400-500mg magnesium
If consuming 1,200mg calcium daily → aim for 400-600mg magnesium
Prioritize DIETARY sources of both (provides natural balance)
If supplementing calcium, ensure adequate magnesium (supplement if dietary intake insufficient)
Signs of Imbalance
Excess calcium, insufficient magnesium:
Muscle cramps, tension
Constipation
Possible increased cardiovascular calcification risk
Excess magnesium, insufficient calcium:
Diarrhea (most common magnesium side effect)
Muscle weakness
Rare with typical intakes (magnesium deficiency much more common than excess)
Vitamin D: The Essential Partner
Evidence quality: VERY STRONG for vitamin D's role in calcium absorption and bone health
Why Vitamin D is Critical
Calcium absorption:
Vitamin D stimulates intestinal calcium absorption
Without adequate vitamin D, you absorb only 10-15% of dietary calcium
With adequate vitamin D, absorption increases to 30-40%
Calcium supplementation without adequate vitamin D is largely ineffective
Bone health effects:
Maintains blood calcium levels (reducing need to pull from bones)
Directly affects bone remodeling (osteoblast and osteoclast function)
Reduces parathyroid hormone (PTH) levels (elevated PTH increases bone resorption)
Evidence:
Vitamin D deficiency causes rickets (children), osteomalacia (adults)
Supplementation with calcium PLUS vitamin D reduces fractures
Vitamin D alone (without calcium) shows modest fracture reduction
Combined supplementation superior to either alone
Vitamin D Requirements for Bone Health
Recommended intakes:
600 IU daily (ages 1-70 years)
800 IU daily (71+ years)
Many experts recommend 1,000-2,000 IU daily for optimal bone health
Optimal blood levels:
25(OH)D (blood test): 30-50 ng/mL (75-125 nmol/L) for bone health
<20 ng/mL considered deficient
20-30 ng/mL insufficient for many people
Sources:
Sunlight (UVB exposure on skin)—varies by latitude, season, skin tone
Fatty fish (salmon, mackerel, sardines)
Fortified foods (milk, plant milks, orange juice, cereals)
Supplements (D3 preferred over D2 for raising blood levels)
Most people require supplementation to achieve optimal levels, especially:
Older adults (reduced skin synthesis)
People with limited sun exposure
Dark skin (requires more sun for same vitamin D production)
Obese individuals (vitamin D sequestered in fat tissue)
Northern latitudes (limited UVB in winter)
Other Nutrients Critical for Bone Health
Evidence quality varies by nutrient
Vitamin K (Evidence: MODERATE to STRONG)
Role in bone:
Required for activation of osteocalcin (bone protein that binds calcium)
May reduce calcium excretion
Appears to improve bone quality
Sources:
Vitamin K1 (phylloquinone): Leafy greens (kale, spinach, collards)
Vitamin K2 (menaquinone): Fermented foods (natto), aged cheese, egg yolks
Supplementation:
Often included in bone health formulas
90-120 mcg daily adequate for most (from diet or supplements)
Caution with warfarin (vitamin K antagonist)
Protein (Evidence: STRONG)
Role in bone:
Provides organic matrix (collagen)
Stimulates IGF-1 (promotes bone formation)
Adequate protein supports muscle mass (reduces fall risk)
Requirements:
At least 0.8g/kg body weight (minimum)
Older adults may need 1.0-1.2g/kg for bone and muscle health
Both animal and plant proteins beneficial
Sources:
Lean meats, poultry, fish
Eggs, dairy
Legumes, tofu, tempeh
Nuts, seeds, whole grains (complementary proteins)
Phosphorus (Evidence: STRONG)
Role in bone:
Major component of hydroxyapatite
~85% of body phosphorus in bones
Balance with calcium:
Typical diet provides adequate phosphorus (often excess from processed foods)
Very high phosphorus with low calcium may be detrimental
Food sources: Dairy, meat, poultry, fish, legumes, nuts
Boron (Evidence: LIMITED to MODERATE)
Role in bone:
May enhance vitamin D and estrogen metabolism
Appears to reduce calcium and magnesium excretion
Sources:
Fruits, vegetables, nuts
Supplementation:
3mg daily may support bone health
Often included in bone formulas
Silicon (Evidence: LIMITED)
Role in bone:
May support collagen synthesis
Associated with bone density in some studies
Sources:
Whole grains, vegetables, beer
Weight-Bearing Exercise: The Essential Component
Evidence quality: VERY STRONG
Why Exercise is Critical
Mechanical loading stimulates bone formation:
Bones respond to stress by becoming stronger (Wolff's Law)
Osteocytes sense mechanical strain
Triggers increased osteoblast activity (bone formation)
Nutrition alone cannot build bone density—mechanical stress required
Types beneficial for bones:
Weight-bearing aerobic:
Walking, jogging, running
Dancing, aerobics
Hiking, stair climbing
Tennis, basketball
Resistance training:
Free weights, weight machines
Resistance bands
Body weight exercises (push-ups, squats, lunges)
High-impact (most effective for bone density, if appropriate):
Jumping, hopping
Running
Sports with running/jumping
NOT appropriate for people with osteoporosis (fracture risk)
NOT weight-bearing (cardiovascular benefits but minimal bone benefits):
Swimming, water aerobics (buoyancy removes weight-bearing)
Cycling
Recommendations:
Weight-bearing exercise: 30 minutes most days
Resistance training: 2-3 days weekly
Include balance and flexibility (reduce fall risk)
Evidence:
Exercise increases bone density in children/adolescents (building peak bone mass)
Maintains bone density in adults
Slows bone loss in older adults
Reduces fracture risk (stronger bones plus reduced falls from improved balance/strength)
Comprehensive Bone Health Strategy
Evidence quality: VERY STRONG for comprehensive approach
Building Peak Bone Mass (Children, Adolescents, Young Adults)
Critical period: Birth to age 30
Nutrition:
Adequate calcium (1,300mg daily ages 9-18—CRITICAL!)
Adequate vitamin D (600-1,000 IU daily or more if deficient)
Adequate protein, magnesium, other bone nutrients
Balanced diet with vegetables, fruits, whole grains, lean proteins, dairy or fortified alternatives
Forever Daily provides baseline comprehensive nutrition supporting bone development
Forever Calcium with vitamin D if dietary calcium insufficient (ensuring absorption optimized)
Exercise:
Weight-bearing and high-impact activities (running, jumping, sports)
Resistance training as appropriate for age
Build habits that continue into adulthood
Lifestyle:
Avoid smoking (reduces peak bone mass)
Limit excessive alcohol
Maintain healthy weight (underweight reduces bone mass)
Maintaining Bone Health (Adults 30-50)
Nutrition:
Continue adequate calcium (1,000mg daily)
Adequate vitamin D (1,000-2,000 IU daily or test and supplement to optimal levels)
Magnesium 400-420mg (men), 310-320mg (women)
Adequate protein, vitamin K
Forever Daily for comprehensive daily nutrition foundation
Forever Calcium if dietary calcium intake falls short of targets
Exercise:
Continue weight-bearing and resistance training
Maintain muscle mass (supports bones, reduces fall risk)
Lifestyle:
Don't smoke
Moderate alcohol if any
Maintain healthy weight
Manage chronic conditions affecting bones (hyperthyroidism, celiac, etc.)
Preventing Bone Loss (Postmenopausal Women, Older Adults)
Highest risk period
Nutrition:
Calcium 1,200mg daily (women post-menopause and adults 71+)
Vitamin D 1,000-2,000 IU daily minimum (higher doses if deficient—common in elderly)
Magnesium 400-420mg (men), 320mg (women)
Adequate protein 1.0-1.2g/kg (higher needs with aging)
Consider vitamin K supplementation
Forever Calcium provides balanced calcium-magnesium-vitamin D support addressing multiple needs
Forever Daily ensures comprehensive nutrition including often-deficient nutrients in elderly (vitamin D, B12, minerals)
Exercise:
Weight-bearing exercise most days
Resistance training 2-3x weekly (maintain muscle and bone)
Balance exercises (tai chi, yoga—reduce fall risk)
Avoid high-impact if osteoporosis diagnosed (fracture risk)
Medical:
Bone density screening (DEXA scan) for women 65+, men 70+, or earlier if risk factors
Fracture risk assessment (FRAX calculator)
Vitamin D testing (many elderly deficient)
Consider medications if osteoporosis diagnosed (bisphosphonates, denosumab, others)
Lifestyle:
Fall prevention (remove tripping hazards, adequate lighting, grab bars, appropriate footwear)
Vision and hearing checks (impairments increase fall risk)
Medication review (some increase fall risk—sedatives, blood pressure meds causing dizziness)
Frequently Asked Questions
Can I get enough calcium without dairy?
YES, absolutely! While dairy is calcium-rich and well-absorbed, many people thrive with dairy-free diets by incorporating alternative calcium sources consistently. Non-dairy calcium sources: (1) Fortified plant milks (almond, soy, oat, coconut)—check labels, most fortified varieties provide 300-450mg per cup (equivalent to cow's milk). Shake well before pouring (calcium settles!). (2) Fortified orange juice—300mg per cup. (3) Leafy greens—cooked collards (268mg/cup), turnip greens (197mg/cup), bok choy (158mg/cup), kale (94mg/cup). NOTE: Spinach, beet greens, Swiss chard are HIGH in oxalates which bind calcium (absorption <5%), so don't count these toward calcium intake despite mineral content. (4) Canned fish with edible bones—sardines (325mg per 3 oz), salmon with bones (180mg per 3 oz). (5) Calcium-set tofu (check labels—varies 250-750mg per half cup depending on brand/type). (6) Fortified foods—cereals, breads (check labels). (7) Legumes—white beans (161mg/cup), chickpeas, black beans (moderate amounts). (8) Nuts and seeds—almonds (75mg/oz), tahini (128mg per 2 tbsp). Practical dairy-free day: Fortified plant milk with cereal (450mg), fortified orange juice (300mg), large collard greens serving at lunch (270mg), tofu stir-fry at dinner (400mg), almonds snack (75mg) = ~1,495mg—supplement additional 300-500mg if needed to reach 1,000-1,200mg target. Key: Be INTENTIONAL and CONSISTENT. Dairy provides concentrated calcium making it easy to reach targets—without it, you must actively include calcium-rich foods at multiple meals daily. Many vegans/dairy-free eaters DO need supplementation to reach optimal intake (nothing wrong with this!). Also ensure adequate vitamin D (often fortified in plant milks but check labels).
Is calcium supplementation safe for my heart?
This is COMPLEX question with nuanced answer. Some studies suggest HIGH-DOSE calcium supplements (>1,000mg daily, particularly calcium carbonate in single doses, WITHOUT adequate vitamin D or magnesium) may modestly increase cardiovascular events (heart attack, stroke) in SOME populations—especially older adults, people with pre-existing cardiovascular disease. Proposed mechanism: Large boluses of supplemental calcium may cause temporary spikes in blood calcium, potentially promoting arterial calcification or blood clotting. HOWEVER: (1) Evidence is MIXED—not all studies show harm, and some show no association. (2) DIETARY calcium does NOT show these cardiovascular concerns—appears safe and beneficial for heart health. (3) Calcium WITH vitamin D in studies often shows neutral or beneficial cardiovascular effects. (4) Vitamin K2 may help direct calcium to bones and away from arteries. Current expert recommendations: (1) PRIORITIZE DIETARY CALCIUM over high-dose supplements when possible—aim to get 800-1,000mg from food, supplement only the gap if needed. (2) If supplementing: Use LOWER doses (500mg or less per dose), take WITH meals (improves absorption, reduces blood calcium spikes), ALWAYS combine with adequate vitamin D (1,000-2,000+ IU daily), ensure adequate magnesium (helps calcium metabolism), consider vitamin K2 (may reduce arterial calcification). (3) Don't EXCEED calcium needs thinking "more is better"—aim for RDA (1,000-1,200mg total from food + supplements), not mega-doses. (4) Divide doses (if taking 1,000mg supplemental, split into 500mg twice daily rather than all at once). (5) Consider calcium citrate over carbonate (absorbed more gradually). Bottom line: DIETARY calcium universally considered safe and beneficial. Supplementation at MODERATE doses (500mg daily or less) with vitamin D, magnesium, and good overall nutrition appears safe for most people. VERY HIGH DOSE supplements (>1,000mg daily) especially without cofactors have potential cardiovascular concerns in some individuals. Work with healthcare provider to assess YOUR specific situation, especially if cardiovascular disease history.
How much magnesium should I take with calcium?
The calcium-magnesium balance is important but individual needs vary. General guidance: Traditional recommendation approximately 2:1 calcium to magnesium ratio based on bone composition and typical dietary patterns. Practical application: (1) If consuming 1,000mg calcium daily (food + supplements combined) → aim for 400-500mg magnesium. (2) If consuming 1,200mg calcium daily → aim for 400-600mg magnesium. (3) Many Americans get TOO MUCH calcium (especially with fortified foods and supplements) but TOO LITTLE magnesium (processed diets low in nuts, seeds, whole grains, leafy greens). This creates ratios of 4:1, 5:1, or higher—potentially problematic. Some experts now suggest: For people consuming HIGH calcium (>1,200mg especially from supplements), consider approaching 1:1 ratio or at minimum 2:1 to ensure adequate magnesium. Example balanced approaches: Approach 1 (moderate calcium, balanced ratio): 1,000mg calcium (600mg from food, 400mg supplement) + 400mg magnesium (200mg from food, 200mg supplement) = 2.5:1 ratio ✓. Approach 2 (higher calcium needs, still balanced): 1,200mg calcium (700mg from food, 500mg supplement) + 500mg magnesium (250mg from food, 250mg supplement) = 2.4:1 ratio ✓. RED FLAG approach (common but problematic): 1,500mg calcium (mostly supplements) + 150mg magnesium (minimal dietary attention) = 10:1 ratio ✗—may impair magnesium function, contribute to muscle cramps, constipation. Dosing magnesium supplements: Start with 200mg daily (magnesium glycinate or citrate), increase to 300-400mg if needed based on dietary intake and total calcium consumption. Take WITH calcium supplement if timing together (don't need to separate), WITH meals to reduce GI effects. Signs you may need more magnesium: Muscle cramps (especially leg cramps at night), eyelid twitching, constipation (if taking calcium supplements), poor sleep. Individual variation matters: Some people need more magnesium relative to calcium (especially those with chronic stress, intense exercise, high calcium supplementation). Others do fine with lower magnesium if dietary calcium moderate. Test if unsure: Can check RBC magnesium (more accurate than serum magnesium) though not commonly done. Bottom line: Don't obsess over EXACT ratios, but ensure you're getting ADEQUATE amounts of BOTH minerals—most people meeting calcium targets but falling short on magnesium. Aim for approximately 2:1 as general guideline, adjust based on individual needs.
When is the best time to take calcium and magnesium supplements?
Timing can affect absorption and side effects. Calcium considerations: (1) Calcium carbonate: MUST take WITH meals (requires stomach acid for absorption). Taking on empty stomach drastically reduces absorption. (2) Calcium citrate: Can take with OR without food (doesn't require acid). Flexibility advantage. (3) Divide doses: Absorption efficiency decreases as dose increases. Take no more than 500-600mg calcium per dose. If supplementing 1,000mg daily, split into 500mg twice (morning with breakfast, evening with dinner). (4) Avoid taking with: Iron supplements (compete for absorption—separate by 2+ hours if taking both), High-fiber meals (may slightly reduce absorption though not dramatically), Thyroid medication (separate by 4 hours—calcium interferes significantly). Magnesium considerations: (1) Take WITH meals: Reduces GI side effects (nausea, diarrhea), improves absorption. (2) Evening dosing may help sleep: Magnesium has mild relaxing effects. Many people take magnesium before bed (may improve sleep quality, reduce leg cramps at night). (3) Avoid taking with: Bisphosphonates (osteoporosis medications—separate by 2+ hours), Certain antibiotics (tetracyclines, quinolones—separate by 2+ hours). Taking calcium and magnesium together: FINE to take together—don't need to separate. Can combine in single dose with meal. Sample timing schedules: Schedule 1 (twice daily): Morning with breakfast: 500mg calcium (carbonate or citrate) + 200mg magnesium. Evening with dinner: 500mg calcium + 200mg magnesium. Total: 1,000mg calcium, 400mg magnesium split across two doses. Schedule 2 (evening focus for magnesium sleep benefits): Morning with breakfast: 500-600mg calcium carbonate. Evening with dinner or before bed: 300-400mg magnesium glycinate (potentially supporting sleep). Schedule 3 (calcium citrate flexibility): Anytime with or between meals: 500mg calcium citrate (morning), 500mg calcium citrate (evening). Evening: 300-400mg magnesium (before bed for sleep support). What to avoid: Taking entire daily calcium dose at once (>600mg)—absorption inefficient. Taking calcium or magnesium on completely empty stomach if prone to GI upset. Taking calcium close to thyroid medication or iron supplements. Bottom line: WITH meals (especially calcium carbonate), DIVIDED doses (calcium especially), CONSISTENT timing (build routine), EVENING magnesium if seeking sleep benefits. Flexibility exists especially with calcium citrate, but meal-timing generally optimal for both absorption and tolerance.
Can I reverse osteoporosis with calcium and magnesium?
Honest answer: Calcium and magnesium alone typically CANNOT reverse established osteoporosis, BUT they are ESSENTIAL components of comprehensive treatment that CAN improve bone density and reduce fracture risk significantly. Understanding osteoporosis reversal: (1) "Reversal" meaning improvement: Increasing bone density from osteoporotic range (T-score ≤ -2.5) to osteopenic range (T-score -1 to -2.5) or higher is POSSIBLE with comprehensive approach including medications. Complete return to normal bone density (T-score > -1) is LESS common but achievable in some cases, especially if caught relatively early. (2) Nutrition alone usually insufficient: Once osteoporosis is established (significant bone loss already occurred), calcium/magnesium/vitamin D typically can SLOW further loss and support bone quality but rarely INCREASE density substantially without medications. (3) Medications often necessary: Bisphosphonates (alendronate, risedronate), denosumab, or anabolic agents (teriparatide, romosozumab) have STRONG evidence for increasing bone density in osteoporosis. These work BY DIFFERENT MECHANISMS than nutrition (directly inhibiting osteoclasts or stimulating osteoblasts). Comprehensive approach (evidence-based): Essential nutrition (foundation): Calcium 1,200mg daily (food + supplements), Vitamin D to achieve blood levels 30-50 ng/mL (often requires 2,000-4,000+ IU daily in deficient individuals), Magnesium 400-500mg daily, Adequate protein 1.0-1.2g/kg body weight, Vitamin K 90-120 mcg daily. Medications (when indicated): Bisphosphonates or other osteoporosis medications as prescribed—these provide the PRIMARY bone density increases in established osteoporosis. Nutrition supports medication effectiveness. Weight-bearing exercise: Essential for bone remodeling stimulus—nutrition provides building blocks but mechanical stress required for formation. Resistance training 2-3x weekly, weight-bearing aerobic activity most days, balance training (fall prevention). Lifestyle: No smoking (impairs bone formation), Minimal alcohol, Fall prevention strategies, Treat underlying conditions (vitamin D deficiency, hyperthyroidism, celiac, etc.). Realistic expectations: (1) With COMPREHENSIVE approach (medications + nutrition + exercise): Many people see 5-15% bone density INCREASES over 2-3 years. Some achieve reclassification from osteoporosis to osteopenia. (2) With NUTRITION/EXERCISE ALONE (no medications): Most people STABILIZE bone density (stop losing) or see MODEST improvements 1-3%. This is valuable (preventing further loss!) but typically doesn't reverse established osteoporosis. (3) Individual variation significant: Younger postmenopausal women respond better than very elderly. Early osteoporosis (T-score -2.6) more reversible than severe (T-score -4.0). Compliance with all interventions critical. Bottom line: Calcium, magnesium, vitamin D, protein, exercise are ESSENTIAL for bone health and should be optimized in everyone with osteoporosis. However, established osteoporosis usually requires MEDICATIONS to achieve significant density increases and fracture risk reduction. Think of nutrition as FOUNDATION that medications and exercise build upon—all three necessary for best outcomes. Work with healthcare provider for personalized treatment plan including bone density monitoring to track progress.
Should children take calcium and magnesium supplements?
MOST children should get calcium and magnesium from FOOD rather than supplements, BUT supplementation may be appropriate in specific situations. Why food first for children: (1) Whole foods provide synergistic nutrients: Dairy and fortified foods provide calcium PLUS protein, vitamin D, phosphorus, vitamin B12. Vegetables, nuts, whole grains provide magnesium PLUS fiber, other minerals, phytonutrients. (2) Establishes healthy eating patterns: Learning to eat nutrient-rich foods builds lifelong habits. Relying on supplements doesn't teach food-based nutrition. (3) Prevents excessive intake: Children's calcium needs LOWER than adults (700-1,300mg depending on age). Easy to over-supplement. (4) Absorption often better from food: Especially for calcium. Calcium needs for children: Ages 1-3: 700mg daily, Ages 4-8: 1,000mg daily, Ages 9-18: 1,300mg daily (CRITICAL bone-building period!). Magnesium needs: Ages 1-3: 80mg daily, Ages 4-8: 130mg daily, Ages 9-13: 240mg daily, Ages 14-18: 360-410mg daily. When supplementation may be appropriate: (1) Dairy allergy or severe lactose intolerance: If child cannot tolerate dairy and family struggles to provide adequate calcium from fortified foods/vegetables consistently. (2) Restrictive eating (picky eaters): Child refuses most calcium-rich foods despite repeated exposure. (3) Vegan diet: Requires attention to fortified plant milks, tofu, vegetables—supplementation may help ensure adequacy. (4) Medical conditions: Celiac disease, IBD, cystic fibrosis, chronic kidney disease (under medical supervision). (5) Medications interfering with absorption: Chronic corticosteroids (under medical supervision). Dosing if supplements needed: Provide only the GAP between dietary intake and needs (not full RDA if getting some from food). Example: Child age 10 consuming ~700mg calcium from food, needs 1,300mg → supplement 300-600mg to close gap (not full 1,300mg causing excess). Use chewable or liquid forms appropriate for age. Give with meals for better absorption and tolerance. Better approach for most children: (1) Ensure 2-3 servings calcium-rich foods daily: Dairy (milk, yogurt, cheese) OR fortified plant milks (shake well!), Fortified orange juice, Calcium-rich vegetables with meals. (2) Include magnesium-rich foods: Whole grain cereals and breads, Nut butters (if no allergy—peanut butter, almond butter), Beans and legumes, Bananas, Dark chocolate (small amounts!). (3) Ensure adequate vitamin D: 600 IU daily from fortified milk/plant milks, fortified cereals, and/or supplement (many children need supplementation especially in winter/northern latitudes). (4) Encourage physical activity: Weight-bearing and impact activities (running, jumping, sports) critical for building peak bone mass during childhood/adolescence. Nutrition alone insufficient! Consult pediatrician: Before starting supplements, discuss with child's doctor to assess actual needs, review diet, and determine appropriate supplementation if truly needed. Bottom line: FOOD FIRST for most children. Supplementation as TARGETED intervention when dietary approaches insufficient despite best efforts, medical conditions present, or restrictive diets make adequacy difficult. Always combine with physical activity for optimal bone development.
Conclusion
Bone health is foundational to lifelong vitality, mobility, and independence, yet over 54 million Americans have osteoporosis or low bone density, placing them at increased fracture risk with potentially devastating consequences. The good news: bone health is largely under our control through nutrition, exercise, and lifestyle choices implemented consistently across the lifespan.
Calcium is the primary structural mineral in bones, with 99% of body calcium stored in the skeleton. Evidence for calcium's bone health benefits is VERY STRONG when combined with adequate vitamin D, showing increased bone density and 15-30% fracture risk reduction in studies. However, calcium alone is insufficient—vitamin D is essential for absorption (without it, you absorb only 10-15% of dietary calcium), and magnesium is required for calcium metabolism and vitamin D activation. Optimal daily intake: 1,000-1,200mg calcium depending on age and gender, prioritizing DIETARY sources (dairy, fortified foods, leafy greens, fish with bones) over high-dose supplements due to potential cardiovascular concerns.
Magnesium, with 50-60% of body stores in bone, has MODERATE to STRONG evidence for supporting bone density and reducing fracture risk. It's required for vitamin D metabolism, parathyroid hormone function, and regulation of bone remodeling. Yet most Americans consume inadequate magnesium (average intake below RDA). Optimal intake: 310-420mg daily depending on age and gender, from nuts, seeds, whole grains, dark leafy greens, legumes, with supplementation (200-400mg magnesium glycinate or citrate) if dietary intake insufficient.
The calcium-magnesium balance matters, with optimal ratio approximately 2:1. Many Americans consume excess calcium (especially with supplements/fortified foods) but inadequate magnesium, creating ratios of 4:1 or higher—potentially problematic. Ensure adequate amounts of BOTH minerals rather than focusing exclusively on calcium.
Vitamin D is the essential partner—without adequate levels (30-50 ng/mL blood 25(OH)D), calcium supplementation is largely ineffective. Most people require 1,000-2,000+ IU daily supplementation to achieve optimal levels. Other important nutrients include vitamin K (bone protein activation), protein (organic matrix, muscle support), and adequate overall nutrition.
Weight-bearing exercise is CRITICAL—nutrition provides building blocks, but mechanical stress is required to stimulate bone formation. Combine weight-bearing aerobic activity, resistance training, and balance exercises. Exercise builds peak bone mass in youth, maintains density in adulthood, and slows loss in older age while reducing fall risk.
Build lifelong bone health today: Optimize calcium intake (1,000-1,200mg daily from food preferably, supplement gap if needed with 500mg doses taken with meals—Forever Calcium provides balanced support with vitamin D and magnesium), ensure adequate magnesium (400-500mg daily from nuts/seeds/whole grains/greens, supplement 200-400mg if dietary intake insufficient), achieve optimal vitamin D levels (test and supplement to 30-50 ng/mL, typically 1,000-2,000+ IU daily—Forever Calcium includes vitamin D, Forever Daily provides additional D3 support), consume adequate protein (0.8-1.2g/kg body weight), include vitamin K-rich foods (leafy greens, fermented foods—Forever Daily includes vitamin K), engage in weight-bearing and resistance exercise (most days, 30+ minutes—builds peak mass in youth, maintains density in adults, slows loss in elderly, reduces falls), don't smoke (impairs bone formation), limit alcohol (excess increases bone loss), maintain healthy body weight (underweight increases osteoporosis risk), get bone density screening when appropriate (women 65+, men 70+, earlier if risk factors), work with healthcare provider (comprehensive assessment, fracture risk evaluation, medications if osteoporosis diagnosed), consider Forever Calcium and Forever Daily for convenient comprehensive bone health support addressing calcium, magnesium, vitamin D, and other essential nutrients in balanced formulations. Your bones are living tissue responding to what you provide them—invest in evidence-based comprehensive bone health for lifelong strength and mobility.
Sources and References
National Osteoporosis Foundation. "Bone Health Guidelines and Research." https://www.nof.org/
Journal of Bone and Mineral Research. "Calcium, Magnesium, and Bone Health." https://asbmr.onlinelibrary.wiley.com/journal/15234681
National Institutes of Health Office of Dietary Supplements. "Calcium and Magnesium Fact Sheets." https://ods.od.nih.gov/
Osteoporosis International. "Clinical Research on Bone Mineral Density." https://link.springer.com/journal/198
American Journal of Clinical Nutrition. "Calcium and Magnesium Metabolism." https://academic.oup.com/ajcn
Bone. "Bone Biology and Mineral Metabolism." https://www.journals.elsevier.com/bone
Journal of Clinical Endocrinology & Metabolism. "Vitamin D and Bone Health." https://academic.oup.com/jcem
About the Author
Naddy is a wellness enthusiast and content creator behind Wellness With Forever. She focuses on simple, practical tips to support a healthy lifestyle through nutrition, movement, and mindful habits.
Disclaimer
This information is for educational purposes only and does not replace professional medical care. Osteoporosis and bone health disorders require professional diagnosis and treatment. Very high calcium supplementation may increase cardiovascular risk. Magnesium supplements interact with medications. Some people should not take calcium supplements without medical supervision. Bone health requires comprehensive assessment including bone density testing and screening for underlying conditions. Always consult healthcare providers before starting supplements, especially if you have medical conditions or take medications.
About Us
Follow
© 2025. WellnessWithForever
SUBSCRIBE